5 Pritchatts Road, Edgbaston, Birmingham B15 2QU
Tel: 0121 687 8882 • Fax: 0121 687 8883
Dental Implants FAQ
This is a Fact Sheet containing Frequently Asked Questions about Dental Implants at the University Dental and Implant Centre. (updated June 2012).
For more information about cost of treatment, please see our private dental care fee scale. We also offer NHS dental treatment to specific groups of people.
- What are implants?
- Why do we need to replace missing teeth?
- What are the advantages over conventional replacements?
- Are implants dangerous to health?
- Can anyone have Implants?
- Is there an age limit to implants?
- What guarantee do we have and what is the success rate?
- What are the known complications?
- Can implants improve my appearance?
- What is the actual procedure?
- What is bone grafting associated with implants?
- How long does the procedure take?
- What should I expect during surgery?
- How much do implants cost?
- Who will carry out the procedure?
- What is the next step?
What are implants?
Implants are specially made posts that replace the roots of teeth that are missing and are used to support a new crown, fixed bridge or denture. It is made of titanium, a strong and lightweight material which has been shown to be compatible with the body and safe for use.
![[Missing Tooth]](/img/treatments/dental-implants/implant1.gif)
Missing Tooth
![[Gap filled with implant without filing good teeth]](/img/treatments/dental-implants/implant2.gif)
Gap filled with implant without filing good teeth
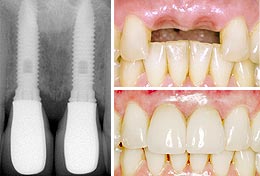
2 Implants for 2 missing front teeth
![[Diagram of an implant with a crown on top]](/img/treatments/dental-implants/implant-with-crown-diagram.jpg)
Diagram of an implant with a crown on top
![[Missing Tooth]](/img/treatments/dental-implants/implant1.gif) Missing Tooth |
![[Gap filled with implant without filing good teeth]](/img/treatments/dental-implants/implant2.gif) Gap filled with implant without filing good teeth |
 2 Implants for 2 missing front teeth |
![[Diagram of an implant with a crown on top]](/img/treatments/dental-implants/implant-with-crown-diagram.jpg) Diagram of an implant with a crown on top |
Why do we need to replace missing teeth?
Our teeth are an important part of our digestive system as it is needed for chewing food. It plays a role in speech. It is also an important part of our appearance. Finally, it prevents gaps and spaces from appearing between our teeth when a tooth is lost.
What are the advantages over conventional replacements?
The conventional methods of replacing missing teeth are Bridges or Dentures.
Bridges usually involve sticking false teeth onto our existing teeth. This may involve filing down healthy teeth to act as retainers which may compromise the health of these teeth. Bridges can also only be provided when there are sufficient strong remaining teeth. They are however a permanent replacement, although they are likely to need replacement every 10 to 15 years.
Dentures are teeth attached to a plastic or metal plate. They can often be cumbersome as they have to be taken in and out every day and for cleaning. They may not always retain in place well if the shape of the gums and bone in the mouth is not appropriate.
Though bridges and dentures can serve us satisfactorily, Implants provide better support and usually results in more comfortable and stable replacement teeth. It provides better chewing efficiency and allows us to have permanent fixed teeth without trimming our own natural teeth for support, or having to remove the teeth every day. Implants also slow down the shrinkage of our jawbone which occurs as a result of tooth loss.
Are implants dangerous to health?
The materials used chiefly titanium is almost never rejected by the body. These have also never been a report of it being the cause of cancer or any life-threatening disease.
Can Anyone Have Implants?
Unfortunately, just having missing teeth does not automatically qualify someone to have dental implants. Some of the criteria that we need to look at are:
Is the patient’s general health satisfactory? There are several medical risk factors against providing dental implants. The most common of these are smoking and diabetes. This does not mean implants cannot be provided in these patients, but the risks of failure are higher and patients need to have this pointed out. However patients with some of these risk factors can also have implants successfully if they can clean their teeth and gums very meticulously.
What is the general condition of the mouth? The remainder of the teeth and gums needs to be stable in order to put in dental implants which are likely to work. If there are other areas of the mouth with dental decay, broken teeth, or gum disease these will need to be treated first before implants are placed. We will give you an idea of other work that may be needed in order to make the mouth stable. Placing implants in a mouth where there are other untreated dental problems can be a recipe for disaster.
Can the patient maintain a healthy mouth? The success of implants can depend on the ability of the patient to keep their teeth and gums clean. We need to be sure this will take place before implants are placed. We will always advise you on how to care for your mouth to allow you to have implants, and also how to care for your new teeth. Your commitment will be to follow our advice. Patients with other medical risk factors can often have implants successfully if they can maintain a very healthy mouth.
Is there sufficient quantity and quality of bone present to allow implants to be placed? Without the right amount of bone in the right place, it is difficult to place implants. Our diagnostic process will help to determine the availability of bone. This is usually done with the help of x-rays. In some cases, we may use a CT-type scan to obtain a 3-dimensional image for more accurate bone assessment. In cases where sufficient bone is not available a range of grafting techniques can be used.
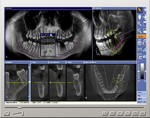
CT Scan Image
![[CT Scan Image: Close-up of jaw]](/img/treatments/dental-implants/opg.jpg)
Close-up of jaw
 CT Scan Image |
![[CT Scan Image: Close-up of jaw]](/img/treatments/dental-implants/opg.jpg) Close-up of jaw |
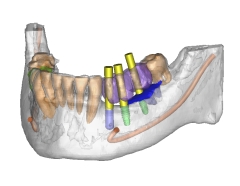
A 3-dimensional image of a lower jaw used to plan implants
These are some of the many factors which we look at in the assessment process. We believe that a thorough assessment gives the best chance of a successful result.
Is there an age limit to implants?
You can be too young for implants but age itself is not a barrier. The state of your health is an important criteria and your dentist will determine your suitability for surgery. After general health the most important criteria is probably whether there is sufficient quality and quantity of bone to accommodate implants. Our dentists will assess this and advise if you are suitable. Contrary to what many people believe, (relative) old age alone is not a barrier to having dental implants.
What guarantee do we have and what is the success rate?
Though no one can ever guarantee success, the procedure has been very well tested and has a success rate of 90-95% in general. Some implants have been monitored for more than 30 years. There will be a need for minor re-servicing from time to time even in successful implants. This is so especially for the denture or fixed teeth which it carries. The success rates given for implants are often thought to be a higher success rate than other treatments such as root canal treatments.
What are the known complications?
As in all surgical procedures there are reported complications. In Implant Dentistry these are mainly either due to a failure of the implant to integrate with the jaw bone, or due to damage to adjacent anatomical structures. The incidence of these complications is very small, and with careful pre-operative planning the risks are kept to an absolute minimum. Here at the University Dental and Implant Centre, we take great care in assessing every case very carefully, discussing with patients the different options, likelihood of success and any related risks.
Where an implant does not integrate with bone, this is sometimes due to a patient having an unfavourable bone pattern or the presence of pre-existing pathology or infection. Often, the site can be left to heal for a few months and the implant successfully reinserted.
Occasionally implants can still fail after several years of having worked well. There may be several reasons for this; one of the most common reason is overloading of implants due to either an insufficient number of implants in the first place (the patient may have insisted on fewer implants than ideal to save costs), or too much stress being placed on the implants on account of a patient’s habit of excessively grinding or clenching their teeth. Again, a thorough assessment and appropriate treatment plan is essential to minimise risks.
Can implants improve my appearance?
Though the main reason for placing implants is to improve our chewing abilities, our teeth play an important part in our appearance and implants can likewise play a role to enhancing our appearance. Do discuss with your dentist as to the cosmetic improvements which are possible as well as the limitations of the procedures. Implants can play a vital role in a "Smile Make-Over" and we often combine implants for the replacement of missing teeth, with crowns for adjacent teeth to give a completely enhanced new smile.
What is the actual procedure?
A surgical procedure is carried out to bury the implant within the jawbone and allow the body to heal naturally. After about 3-6 months, the implants will be strong enough to support the load of new teeth which is attached to them. During the healing period, you will be provided with temporary "teeth" to allow you to carry on your way of life until the bone completely surrounds the implant. This may be an adhesive-type bridge or a denture. The animation below explains the procedure.
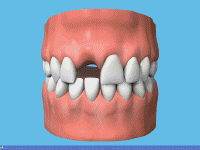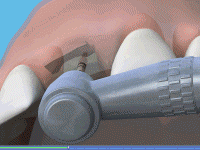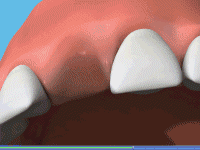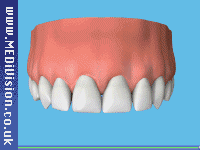
Animation of implant procedure

X-ray showing implant inserted in bone
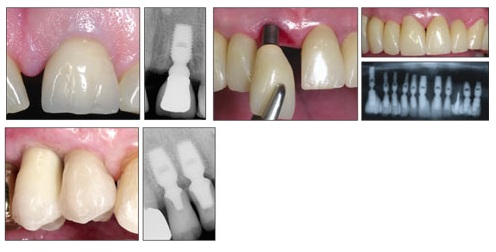
X-ray showing implant inserted in bone
What is bone grafting associated with implants?
Successful placement of implants depends on the presence of bone of sufficient quality and quantity. This is not always present in every patient. A lack of bone is usually related to local factors such as how the gums healed after tooth extraction, rather than any general medical condition.
It was previously thought that in areas where there was insufficient bone it was not possible to place implants. There have now been great advances made in procedures to increase the amount of available bone either by use of endogenous bone (i.e. belonging to the patient) or a range of artificial substitutes or a combination of both. These grafting techniques are simple and often carried out at the time of implant placement. For areas where there is significant lack of bone more complex grafting procedures can also be carried out to restore bone volume.
Here at the University Dental and Implant Centre, we are experienced in these techniques and will discuss with you the best options. We also work with a Consultant Maxillo-Facial Surgeon to carry out complex grafting procedures such as external sinus lifts, block grafting and even iliac crest (hip) grafting.
How long does the procedure take?
This depends largely on complexity but can range from one to two hours per implant. The dentist will advise you of the schedule for the different visits. You might need to take a couple of days off work after the insertion of the implants. Each case will be different and will require inidividual assessments for establishing treatment needs.
What should I expect during surgery?
The procedure is normally carried out under local anaesthesia. For patients who are anxious, intravenous sedation is also offered. During the surgery, the local anaesthesia and sedation given practically eliminates all pain. After the surgery, there will be some discomfort, swelling or bruising but with the appropriate medication, it is usually not unduly uncomfortable. However, it is important to note that different people can heal at different rates.
How much do implants cost?
As materials and techniques used are fairly sophisticated, there is a cost attached to having implants. However, in terms of quality of life, there is definitely a dramatic improvement for the many people across the world that have benefited from this procedure. The University Dental and Implant Centre’s normal charge is £2,500 per tooth including crown provision and post-treatment follow-up. If bone grafting is required, this may add up to £200 per implant for simple grafts. For more complex cases, which may involve additional procedures like sinus lifts, larger grafts or multiple implants, your dentist will discuss the costs. Generally, the unit cost will reduce where more than 3 implants are placed. For example, an approximate cost replacing a full upper set of teeth (usually 10 teeth) is around £10,000-13,000.
CT-type scans to give 3-dimensional imaging can cost around £95 per jaw. We may recommend this in complex cases involving many implants. This type of investigation gives us the most accurate and predictable way of planning complex cases.
Please note: the prices indicated above are only a guide and will depend entirely upon the initial assessment. The normal consultation charge for those who are not registered with the practice is £70, inclusive of all x-rays and investigations.
Who will carry out the procedure?
Here at the University Dental and Implant Centre, dental implants are carried out by the Lead Clinician Dr Abhi Pal with his team of nurses and technicians who are highly experienced in this procedure.
Dr Pal has extensive experience and training in Restorative Dentistry and Dental Implants. He has been carrying out Implant Dentistry at this practice since 1993 and has undergone training courses in implant dentistry in the UK, Sweden and the US. He fully complies with the FGDP Training Standards in Implant Dentistry, as endorsed by the GDC, and is a member of the Association of Dental Implantology.
Dr Pal has worked as part of team at the University of Bristol carrying out out research into the bacteria causing peri-implant disease which has resulted in the following publication:
Molecular analysis of microbiota associated with peri-implant diseases. Al-Radha AS, Pal A, Pettemerides AP, Jenkinson HF. J Dent. 2012 Nov;40(11):989-98
What is the next step?
Arrange an implant consultation with Dr Abhi Pal to assess your mouth. He will make some moulds and take some radiographs and photographs. After doing some planning, he will be able to inform you when you can get started on replacing those missing teeth, and an estimate of the costs.
Copyright © 2002-2024, The University Dental and Implant Centre. All rights reserved. Copyright, Privacy & Accessibility Information.
